Parkinson’s disease is a complex neurodegenerative disorder that significantly impacts the lives of individuals diagnosed with the condition. Characterized by a range of motor and non-motor symptoms, Parkinson’s disease poses challenges to daily functioning, affecting mobility, communication, and overall well-being. While there is currently no cure for Parkinson’s disease, ongoing research is exploring various treatment modalities, including medications, surgical interventions, and lifestyle interventions, to enhance symptom management and improve the quality of life for those affected. Support groups and caregiver networks play a vital role in providing emotional support and valuable insights for individuals navigating the complexities of Parkinson’s disease. In this webpage, we will try to cover most of the aspects relating to Parkinson’s Disease for easy understanding of everyone in a question and answer type format.
Interview in Kannada Language about Parkinson's Disease
Understanding Parkinson's Disease from Nature Publications
Parkinson's Disease Demystified: The Ultimate Guide to Symptoms and Solutions
1. What is Parkinson’s Disease?
Animation of changes happening in Parkinson disease brain
Parkinson’s disease is a health condition that affects the way your body moves. It happens because some parts of your brain, which help control movements, stop working properly. This can lead to problems like shaking or trembling in your hands, stiffness in your muscles, and difficulty moving smoothly. Think of it like a glitch in the communication system between your brain and muscles.
People with Parkinson’s might notice that simple actions, like walking or picking up things, become more challenging. It’s not just about movement – Parkinson’s can also bring about other changes, like trouble sleeping or feeling moody. While there’s no cure, treatments and support can help manage these challenges and improve daily life for those with Parkinson’s.
2. Was Parkinson’s Disease known in ancient medical scriptures?
In ancient medical scriptures, descriptions of conditions resembling symptoms associated with Parkinson’s disease are not explicitly documented in the way we understand the disorder today. However, historical texts from various cultures may contain descriptions of conditions that could be interpreted as having similarities to certain aspects of Parkinson’s disease.
-
Indian Ayurvedic Texts:
– In Ayurveda, as mentioned earlier, the term “Kampavata” is used to describe conditions involving tremors or shaking movements, resembling aspects of Parkinson’s symptoms.
-
Chinese Medicine:
– In traditional Chinese medicine, there may be references to conditions affecting movement or balance, but the terminology and conceptualization would be different from modern medical descriptions of Parkinson’s disease.
-
Ancient Egyptian and Babylonian Medicine:
– Medical practices in ancient Egypt and Babylonia focused on a range of health issues, but specific descriptions resembling Parkinson’s disease are not found in the surviving texts.
-
Greek and Roman Medicine:
– In Greco-Roman medical writings, there might be descriptions of movement disorders, but they would not match the modern understanding of Parkinson’s disease.
It’s important to recognize that the understanding of diseases and their classifications has evolved significantly over time. Ancient medical systems often relied on different conceptual frameworks and lacked the detailed anatomical and physiological knowledge that we have today.
If there were descriptions of conditions resembling Parkinson’s in ancient texts, they would likely be interpreted within the cultural and medical context of those times, using terms and concepts that might not directly align with our contemporary understanding. Interpreting historical medical texts requires a careful consideration of the cultural, linguistic, and medical contexts of the time.
3. What are the Early symptoms of Parkinson’s disease?
Early Symptoms of Parkinson's Disease
The early symptoms of Parkinson’s disease can be subtle and may vary from person to person. Here are some common early signs:
- Tremors: Shaking or trembling in the hands, fingers, or other parts of the body, especially at rest.
- Bradykinesia: Slowness of movement. This can make simple tasks take longer to complete.
- Muscle Stiffness: Stiffness or rigidity of muscles, particularly in the arms, legs, or neck.
- Postural Instability: Difficulty maintaining balance and coordination, which may lead to a higher risk of falls.
- Changes in Handwriting: Known as micrographia, handwriting may become smaller and more difficult to read.
- Reduced Arm Swing: A decreased or absent swinging of the arms when walking.
- Facial Expression Changes: A reduction in facial expressions, often referred to as a “masked face.”
- Soft or Monotone Speech: Changes in speech patterns, such as a softer voice or a lack of modulation.
- Decreased Sense of Smell: Some individuals may experience a loss of or reduced sense of smell.
It’s important to note that not everyone with Parkinson’s disease will experience all of these symptoms, and some may not notice them at all in the early stages. Additionally, these symptoms can be caused by various other conditions, so a thorough medical evaluation is necessary for an accurate diagnosis.
Early Classical Motor Symptoms of Parkinson's Disease - Well known as TRAP features
4. How does a doctor diagnose Parkinson’s disease?
Illustration of Parkinson's disease diagnosis approach
Diagnosing Parkinson’s disease involves a comprehensive evaluation by a healthcare professional, typically a neurologist with expertise in movement disorders. The diagnostic process includes a combination of medical history review, clinical examination, and sometimes additional tests. Here’s an overview of the steps involved in diagnosing Parkinson’s disease:
- Medical History:
– The doctor will inquire about the individual’s medical history, including symptoms, their onset, and any family history of neurological disorders.
- Clinical Examination:
– The neurologist will conduct a thorough physical examination, assessing various aspects such as muscle strength, coordination, reflexes, and posture. They will also observe for specific motor symptoms associated with Parkinson’s disease, including tremors, bradykinesia (slowness of movement), and muscle rigidity.
- Unified Parkinson’s Disease Rating Scale (UPDRS):
– This is a standardized scale used to assess the severity of Parkinson’s symptoms. It includes evaluations of both motor and non-motor symptoms.
- Response to Medications:
– Parkinson’s disease symptoms often respond positively to medications that increase dopamine levels. If the doctor suspects Parkinson’s, they may prescribe a medication such as levodopa to observe the patient’s response.
- Neuroimaging Studies:
– While not mandatory for diagnosis, neuroimaging studies such as MRI or DaTscan may be used to rule out other conditions that can mimic Parkinson’s symptoms.
- Blood Tests:
– Blood tests may be performed to rule out other potential causes of similar symptoms, ensuring a more accurate diagnosis.
- Differential Diagnosis:
– Parkinson’s disease shares symptoms with other conditions, and the doctor will consider alternative diagnoses. Reaching a definitive diagnosis may require multiple evaluations over time.
- Consultation with Specialists:
– In some cases, a doctor may refer the individual to a movement disorder specialist for a more specialized assessment.
It’s important to note that there is no single test that definitively confirms Parkinson’s disease. The diagnosis is often based on a combination of clinical judgment, observation of symptoms, and the exclusion of other possible causes.
How Does DAT Scan help in the diagnosis of Parkinson's disease - an illustration
5. What is the difference between Parkinsonism and Parkinson’s Disease?
“Parkinsonism” is a term used to describe a set of symptoms that resemble those seen in Parkinson’s disease. It is a broad term encompassing various conditions that manifest with similar motor symptoms but may have different underlying causes. Parkinson’s disease is just one of several potential causes of parkinsonism. Parkinson’s disease is a specific and common form of parkinsonism, while parkinsonism is a broader term encompassing various conditions that share similar motor symptoms.
6. What are some examples of Parkinsonism disorders and their features?
Parkinsonism can result from various underlying causes, and there are several disorders and conditions that exhibit parkinsonian symptoms. Here are some examples:
- Parkinson’s Disease (PD):
– As the most common cause of parkinsonism, Parkinson’s disease is a neurodegenerative disorder characterized by the loss of dopamine-producing neurons in the brain.
- Drug-Induced Parkinsonism:
– Certain medications, particularly antipsychotic drugs and antiemetics, can induce parkinsonian symptoms as a side effect. This condition is often reversible once the medication is discontinued.
- Vascular Parkinsonism:
– Caused by multiple small strokes affecting the brain’s blood vessels, vascular parkinsonism leads to parkinsonian symptoms. It may occur suddenly and can be associated with other signs of vascular damage.
- Progressive Supranuclear Palsy (PSP):
– PSP is a rare neurodegenerative disorder that causes problems with walking, balance, and eye movement. It shares some symptoms with Parkinson’s disease but has distinctive features, such as difficulties with eye control.
- Multiple System Atrophy (MSA):
– MSA is a rare neurodegenerative disorder that involves the degeneration of multiple areas of the brain. It can present with parkinsonian symptoms, as well as autonomic dysfunction (blood pressure fluctuations, dizziness, urinary issues) and cerebellar ataxia.
- 6. Corticobasal Syndrome (CBS):
– Corticobasal syndrome is a neurodegenerative disorder characterized by asymmetric motor symptoms, including parkinsonism, along with cognitive (memory) and sensory abnormalities (abnormal hand posturing / movements).
- Lewy Body Dementia (LBD):
– Lewy body dementia is a progressive brain disorder that can cause parkinsonian symptoms, cognitive changes, and hallucinations. It is associated with the presence of Lewy bodies, abnormal protein deposits in the brain.
- Normal Pressure Hydrocephalus (NPH):
– NPH is a condition characterized by the accumulation of cerebrospinal fluid in the brain’s ventricles. It can lead to parkinsonian symptoms, gait disturbances, and urinary incontinence.
It’s important to note that these conditions have distinct features, and the diagnosis of parkinsonism requires a thorough evaluation by a neurologist. Determining the underlying cause is crucial for appropriate treatment and management strategies.
7. What are the Motor symptoms of Parkinson’s disease?
Classical Motor Features of Parkinson's Disease - The TRAP Features
Motor symptoms are a hallmark feature of Parkinson’s disease, and they result from the progressive loss of dopamine-producing neurons in the brain. Here are the primary motor symptoms associated with Parkinson’s disease:
- Tremors:
– Involuntary shaking or trembling of the hands, fingers, or other parts of the body, especially at rest. Tremors often have a rhythmic quality.
- Bradykinesia:
– Slowness of movement. Individuals with Parkinson’s disease may experience a gradual reduction in the ability to initiate and complete movements. Simple tasks may take longer to perform.
- Muscle Rigidity:
– Stiffness or inflexibility of muscles. This can occur in various parts of the body, leading to discomfort and a reduced range of motion.
- Postural Instability:
– Difficulty maintaining balance and an increased risk of falls. People with Parkinson’s disease may have a stooped or forward-leaning posture.
- Akinesia:
– Reduced ability to initiate voluntary movements. Akinesia is closely related to bradykinesia and can contribute to a sense of “freezing” or being unable to start moving.
- Loss of Automatic Movements:
– A decline in automatic movements, such as reduced arm swing while walking or a diminished ability to perform activities that are typically done without conscious thought.
- Micrographia:
– A tendency for handwriting to become smaller and more cramped. This can make written communication challenging.
- Speech Changes:
– Softening of the voice, monotone speech, or other alterations in speech patterns. People with Parkinson’s may speak more slowly or with reduced intonation.
- Dystonia:
– Involuntary muscle contractions that can cause twisting or repetitive movements. Dystonia may affect the hands, fingers, or other body parts.
These motor symptoms can vary in severity from person to person and can change over time. Additionally, not every individual with Parkinson’s disease will experience all of these symptoms. It’s important to note that non-motor symptoms, such as cognitive changes and mood disorders, are also common in Parkinson’s disease. If someone is experiencing these symptoms, it’s crucial to seek medical evaluation for an accurate diagnosis and appropriate management.

Pictorial representation of Motor symptoms (which are easily seen as body of the tree) and Non Motor symptoms (which are not seen and need to be specifically asked for - like the root system of a tree)
8. What do you mean by ‘Non Motor Symptoms (NMS)’ and what are the Non Motor symptoms seen in Parkinson’s Disease?
Video illustration about Non Motor symptoms in Parkinson's disease
Non-motor symptoms (NMS) in Parkinson’s disease refer to a wide range of symptoms that do not directly involve movement but can significantly impact an individual’s overall well-being and quality of life. These symptoms can affect various bodily systems and functions beyond the motor (movement-related) aspects associated with Parkinson’s disease. Here are some common non-motor symptoms in Parkinson’s disease:
- Cognitive Changes:
– Mild Cognitive Impairment: Some individuals may experience difficulties with memory, attention, and other cognitive functions, often referred to as mild cognitive impairment (MCI).
– Dementia: In advanced stages, a significant number of people with Parkinson’s disease may develop dementia, characterized by more pronounced cognitive decline.
- Mood Disorders:
– Depression: Feelings of sadness, hopelessness, and a loss of interest or pleasure in activities.
– Anxiety: Excessive worrying, restlessness, and feelings of unease.
– Apathy: Lack of motivation or interest in activities that were previously enjoyable.
- Sleep Disturbances:
– Insomnia: Difficulty falling asleep or staying asleep.
– REM Sleep Behavior Disorder (RBD): Acting out dreams physically during sleep, which can lead to injuries.
- Autonomic Dysfunction:
– Orthostatic Hypotension: A sudden drop in blood pressure upon standing, leading to dizziness or fainting.
– Constipation: Slowed digestive system, resulting in difficulty passing stool.
– Urinary Problems: Issues with urine retention or urgency.
- Sensory Symptoms:
– Loss of Smell (Hyposmia): A reduced sense of smell is common in Parkinson’s disease.
– Visual Disturbances: Blurred or double vision.
- Pain:
– Musculoskeletal Pain: Pain or discomfort in muscles and joints.
– Neuropathic Pain: Nerve-related pain, such as tingling or burning sensations.
- Fatigue:
– A persistent feeling of tiredness or lack of energy, which is not always relieved by rest.
- Speech and Swallowing Difficulties:
– Changes in speech clarity and difficulties with swallowing, known as dysphagia.
- Psychiatric Symptoms:
– Hallucinations: Seeing, hearing, or sensing things that are not present.
– Delusions: False beliefs or misconceptions.
These non-motor symptoms can significantly impact a person’s daily life and may contribute to a decrease in overall functioning. It’s essential for healthcare professionals to address both motor and non-motor aspects of Parkinson’s disease when developing a comprehensive treatment plan. Individual experiences with non-motor symptoms can vary, and their management often requires a multidisciplinary approach involving neurologists, psychiatrists, physical therapists, and other healthcare professionals.
9. What Causes Parkinson’s Disease?
Causes or Reasons for occurence of Parkinson's disease
The exact cause of Parkinson’s disease is not fully understood, and it is likely influenced by a combination of genetic and environmental factors. Here are key aspects related to the potential causes of Parkinson’s disease:
- Genetic Factors:
– While most cases of Parkinson’s disease are considered sporadic (occurring without a clear family history), there is evidence that genetic factors can contribute.
– Some rare genetic mutations have been linked to familial or early-onset forms of Parkinson’s disease. However, these cases represent a small percentage of overall cases.
- Environmental Factors:
– Exposure to certain environmental factors has been investigated as a potential risk for developing Parkinson’s disease. These factors may include:
– Pesticides and Herbicides: Some studies suggest an association between exposure to certain agricultural chemicals and an increased risk of Parkinson’s.
– Head Trauma: Severe head injuries and trauma may be linked to an increased risk, particularly in some cases of parkinsonism.
– Industrial Toxins: Exposure to certain industrial chemicals, such as solvents and metals, has been explored as a potential risk factor.
- Neurodegeneration and Dopamine Loss:
– Parkinson’s disease is characterized by the progressive degeneration of dopamine-producing neurons in a specific region of the brain called the substantia nigra. The loss of these neurons leads to a reduction in dopamine levels, contributing to the motor symptoms of Parkinson’s.
- Lewy Bodies:
– Lewy bodies are abnormal protein aggregates found in the brains of individuals with Parkinson’s disease. The presence of Lewy bodies is a pathological hallmark of the disease, but their exact role in the development of Parkinson’s is still not fully understood.
- Inflammation and Immune System Involvement:
– There is growing research suggesting that inflammation and immune system responses may play a role in the development of Parkinson’s disease.
It’s important to note that Parkinson’s disease is a complex disorder, and its development likely involves a combination of multiple factors. Additionally, the majority of cases are sporadic, with no clear family history, suggesting that environmental factors and complex interactions between genes and the environment contribute to the risk.
Research is ongoing to better understand the underlying mechanisms of Parkinson’s disease and to identify potential targets for interventions and treatments. As of now, there is no cure for Parkinson’s disease, but treatments are available to manage symptoms and improve the quality of life for individuals with the condition.
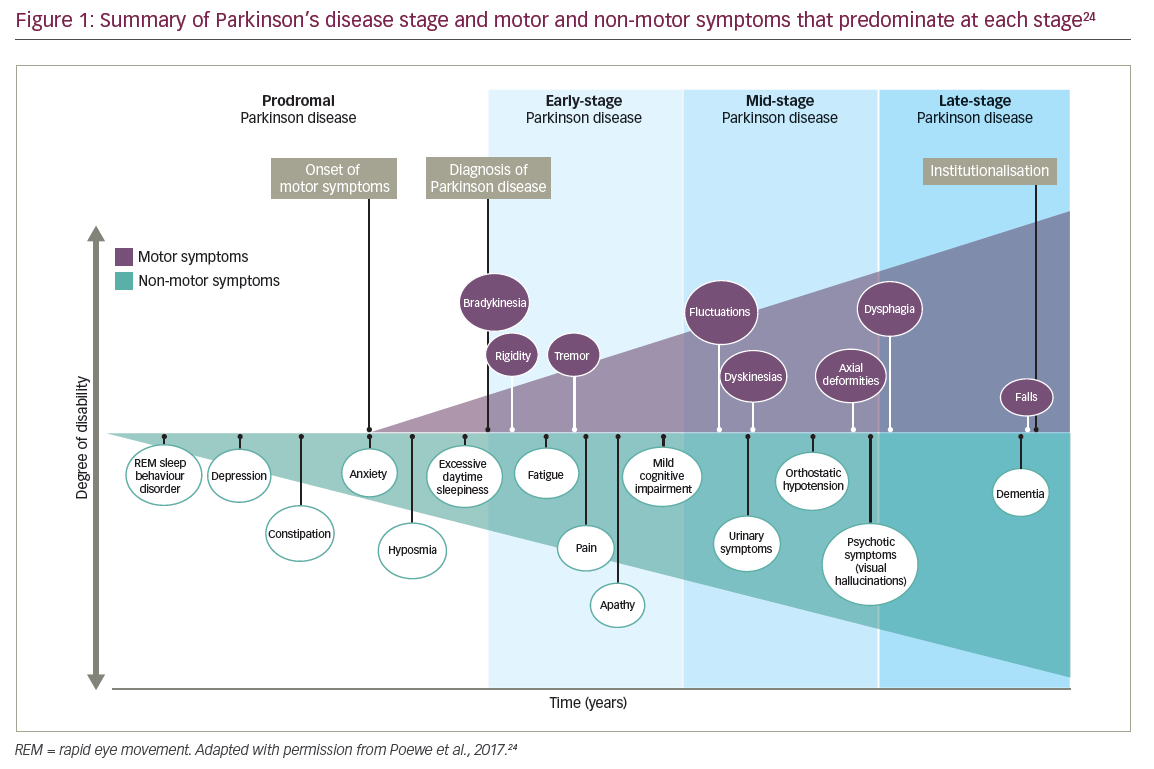
10. What are the different stages of Parkinson’s disease?
Stages of Parkinson's Disease
Parkinson’s disease is often categorized into different stages to help describe the progression of symptoms over time. It’s important to note that these stages provide a general framework, and the progression of the disease can vary widely among individuals. The most commonly used staging system is based on the Hoehn and Yahr Scale and the Unified Parkinson’s Disease Rating Scale (UPDRS). Here is a general overview of the stages:
Stage 1: Early Stage
– Symptoms: Mild and may be subtle.
– Characteristics:
– Tremors or other motor symptoms on one side of the body.
– Minimal or no functional impairment.
– Activities of daily living are not significantly affected.
Stage 2: Mild Stage
– Symptoms: Symptoms become more noticeable and may affect both sides of the body.
– Characteristics:
– Balance is still maintained.
– Daily activities are minimally affected.
– Posture may be affected.
Stage 3: Moderate Stage
– Symptoms: Moderate symptoms with noticeable slowing of movements.
– Characteristics:
– Impaired balance and coordination.
– Functional independence is compromised.
– Falls may occur, but individuals can still manage some activities.
Stage 4: Advanced Stage
– Symptoms: Severe symptoms with a significant impact on daily life.
– Characteristics:
– Limited ability to perform daily activities without assistance.
– Tremors, stiffness, and bradykinesia are pronounced.
– Increased risk of falls.
Stage 5: Severe/End Stage
– Symptoms: Advanced and severe symptoms.
– Characteristics:
– Wheelchair-bound or bedridden.
– Dependent on others for daily care.
– Cognitive decline may be present in some cases.
– Increased susceptibility to complications.
It’s important to emphasize that the progression through these stages is individualized, and not everyone will experience the same rate of decline or exhibit all the listed characteristics. Additionally, advancements in medical treatments and interventions may influence the progression of the disease, providing individuals with better management of symptoms and improved quality of life. Parkinson’s disease is a complex condition, and healthcare professionals tailor treatment plans to address the specific needs of each individual. Regular communication with healthcare providers is essential for monitoring and adjusting the management of Parkinson’s disease as it progresses.
11. Is there a cure for Parkinson’s Disease Or How Parkinson’s disease is treated?
Parkinson's Medications Explained
As of current status in 2024, there is no cure for Parkinson’s disease. However, there are various treatment approaches aimed at managing symptoms, improving quality of life, and enhancing functional abilities. Treatment plans are often individualized based on the specific needs and symptoms of each person with Parkinson’s disease. Here are key components of Parkinson’s disease treatment:
Medications:
- Levodopa (L-dopa): Converts into dopamine in the brain, helping to alleviate motor symptoms. It is often combined with other medications.
- Dopamine Agonists: Mimic the action of dopamine in the brain.
- MAO-B Inhibitors and COMT Inhibitors: Extend the effects of levodopa by preventing its breakdown.
- Anticholinergic Medications: May help control tremors and rigidity in some cases.
Continuous Dopaminergic Infusion Therapies(CDI):
- Role: CDI involves the continuous delivery of a dopamine agonist, usually apomorphine, via a portable infusion pump. This is an option for individuals experiencing fluctuations in motor responses to oral medications.
Deep Brain Stimulation (DBS):
– Surgical procedure involving the implantation of electrodes into specific areas of the brain. These electrodes are connected to a stimulator device, which can help regulate abnormal brain activity and alleviate motor symptoms.
Physical Therapy:
– Exercises and physical activities designed to improve flexibility, strength, balance, and coordination.
Occupational Therapy:
– Focuses on maintaining independence in daily activities through strategies and adaptations.
Speech Therapy:
– Helps address speech and swallowing difficulties that may arise in Parkinson’s disease.
Supportive Therapies:
– Exercise Programs: Regular physical activity has been shown to be beneficial in managing symptoms and improving overall well-being.
– Nutritional Support: A balanced diet can contribute to overall health and may be important for individuals with Parkinson’s disease.
– Psychological Support: Counseling and support groups can help individuals cope with emotional and psychological aspects of the disease.
Research and Clinical Trials:
– Ongoing research aims to understand the underlying mechanisms of Parkinson’s disease and develop new treatment strategies. Participating in clinical trials may provide access to emerging therapies.
It’s important for individuals with Parkinson’s disease to work closely with healthcare professionals to monitor symptoms, adjust medications as needed, and explore appropriate therapies. While there is no cure, advances in research and treatment options continue, providing hope for improved management and, potentially, future breakthroughs in the understanding and treatment of Parkinson’s disease. It’s recommended to stay informed about the latest developments in Parkinson’s research and to consult with healthcare providers for the most up-to-date information.
12. What is the role of complimentary and alternative medicines in management of Parkinson’s disease, including Ayurveda, Yoga, Unnani, Siddha, homeopathy, (AYUSH) traditional Chinese medications?
Complimentary and Alternative Medicine
Complementary and alternative medicines, including those from traditional systems such as Ayurveda, Yoga, Unani, Siddha, homeopathy, and traditional Chinese medicine, are often explored by individuals with Parkinson’s disease as adjunct therapies. It’s important to note that while some people may find these approaches beneficial in managing certain symptoms or improving overall well-being, they should not be considered as substitutes for conventional medical treatments. The effectiveness of these approaches can vary, and individual responses may differ. Here’s an overview of some complementary and alternative therapies often considered in the context of Parkinson’s disease:
- Ayurveda:
– Ayurveda, an ancient Indian system of medicine, may involve herbal remedies, dietary changes, and lifestyle practices.
– Some Ayurvedic herbs and formulations are believed to have neuroprotective properties.
- Yoga:
– Regular yoga practice is associated with improvements in flexibility, balance, and muscle strength.
– Mindful movement and breathing exercises in yoga can contribute to overall well-being.
- Unani:
– Unani medicine, originating from ancient Greece and Persia, may involve herbal remedies, dietary advice, and lifestyle modifications.
– The approach is based on the balance of bodily humors.
- Siddha:
– Siddha medicine, traditional to South India, may include herbal preparations and lifestyle recommendations.
– Certain herbs are believed to have therapeutic properties.
- Homeopathy:
– Homeopathy involves the use of highly diluted substances to stimulate the body’s natural healing processes.
– Individualized treatments based on the person’s specific symptoms are common.
- Traditional Chinese Medicine (TCM):
– TCM includes acupuncture, herbal medicine, dietary recommendations, and exercises like Tai Chi.
– Acupuncture may be used to address specific symptoms, and herbal formulations are tailored to individual needs.
Considerations:
– Individual Responses: Responses to these therapies can vary widely, and what works for one person may not work for another.
– Safety: It’s crucial to discuss the use of complementary and alternative therapies with healthcare providers to ensure they do not interfere with prescribed medications or worsen symptoms.
– Research: Limited scientific evidence supports the effectiveness of these approaches in Parkinson’s disease. Research is ongoing, and findings may evolve over time.
Caution:
– No Cure: These therapies should not be seen as cures for Parkinson’s disease. Conventional medical treatments remain the primary means of managing the condition.
– Consultation: Always consult with healthcare professionals before incorporating complementary or alternative therapies into the treatment plan.
Individuals interested in exploring these approaches should inform their healthcare team, and decisions should be made collaboratively to ensure a comprehensive and safe approach to managing Parkinson’s disease. Regular medical check-ups and open communication with healthcare providers are essential.
13. What is the role of Kapikachu, velvety beans and mucuna pruniens in management of Parkinson’s Disease?

Image of Mucuna Pruriens / Velvet Beans which has good content of Dopamine
Kapikachu, also known as velvet bean or Mucuna pruriens, is an herb that has gained attention in the context of Parkinson’s disease due to its high natural content of levodopa. Levodopa is a medication commonly used in the treatment of Parkinson’s disease to replenish dopamine, a neurotransmitter that is deficient in individuals with the condition. Here is some information about the potential role of Kapikachu in the management of Parkinson’s disease:
Mucuna pruriens (Kapikachu):
– Levodopa Content: Mucuna pruriens contains a significant amount of levodopa, which is a precursor to dopamine. This is the key compound responsible for the therapeutic effects in Parkinson’s disease.
– Natural Source: Unlike synthetic levodopa used in medications, Mucuna pruriens provides levodopa in its natural form, along with other beneficial compounds.
– Antioxidant Properties: Mucuna pruriens has antioxidant properties, which may have neuroprotective effects.
Role in Parkinson’s Disease Management:
- Symptom Relief:
– The levodopa content in Mucuna pruriens can help alleviate motor symptoms associated with Parkinson’s disease, such as tremors, bradykinesia, and muscle stiffness.
- Potential for Reduced Side Effects:
– Some individuals believe that the natural form of levodopa in Mucuna pruriens may lead to fewer side effects compared to synthetic levodopa medications. However, this is a topic of ongoing research.
Important Considerations:
– Variable Levodopa Content: The levodopa content in different preparations of Mucuna pruriens can vary, making it challenging to standardize dosages. This variability may affect the consistency of symptom relief.
– Interaction with Medications: The use of Mucuna pruriens alongside conventional Parkinson’s medications should be carefully monitored, as it can potentially lead to excessive dopamine levels and side effects. Consultation with a healthcare professional is crucial.
– Adverse Effects: While Mucuna pruriens is generally considered safe, some individuals may experience side effects such as nausea, vomiting, or dyskinesias (involuntary movements). Monitoring for adverse effects is important.
– Not a Replacement for Standard Treatment: Mucuna pruriens is not a substitute for prescribed medications for Parkinson’s disease. It should be considered as a complementary or adjunct therapy under the guidance of healthcare professionals.
Research on the use of Mucuna pruriens in Parkinson’s disease is ongoing, and its potential benefits and risks are areas of active investigation. Individuals considering the use of Mucuna pruriens should discuss it with their healthcare team to ensure coordinated and safe management of Parkinson’s disease symptoms. Any adjustments to the treatment plan should be made in consultation with healthcare professionals.
14. What are the infusion therapies and their role in management of Parkinson’s disease?
Media coverage about Duopa - Duodopa Infusion therapy
Infusion therapies, particularly in the context of Parkinson’s disease, typically involve the administration of medications directly into the bloodstream through an intravenous (IV) line. These therapies are often used when oral medications are insufficient in controlling symptoms or when there are challenges with oral medication absorption. Here are some infusion therapies that may be considered in the management of Parkinson’s disease:
- Continuous Subcutaneous Apomorphine Infusion:
– Role: Apomorphine is a dopamine agonist that can be administered continuously through a subcutaneous infusion using a portable pump. This is suitable for individuals with advanced Parkinson’s disease and motor fluctuations.
– Benefits:
– Provides continuous dopaminergic stimulation.
– Reduces “off” periods and improves motor function.
- Duodopa (Carbidopa/Levodopa Enteral Suspension):
– Role: Duodopa is a gel formulation of carbidopa/levodopa administered directly into the small intestine through a surgically placed tube (duodenal or jejunal infusion). It provides a continuous supply of medication throughout the day.
– Benefits:
– Addresses motor fluctuations and “off” periods.
– Improves overall motor symptom control.
– Reduces “off” periods when symptoms are not well controlled.
- Intravenous Levodopa:
– Role: In specific situations, intravenous levodopa may be administered in a hospital setting to address severe motor fluctuations or during episodes of acute worsening of symptoms.
– Benefits:
– Rapid and direct delivery of levodopa to manage acute motor challenges.
Considerations and Limitations:
– Surgical Intervention: Some infusion therapies, such as Duopa, require a surgical procedure for the placement of the infusion tube. The decision to undergo surgery should be made in consultation with healthcare providers.
– Monitoring and Adjustments: Infusion therapies require close monitoring to ensure optimal dosing and to make necessary adjustments based on individual responses and changing symptoms.
– Potential Complications: There can be risks and complications associated with infusion therapies, including infections, pump malfunctions, and device-related issues.
– Individualized Approach: The choice of infusion therapy is often individualized based on the specific needs, preferences, and circumstances of each person with Parkinson’s disease.
Infusion therapies can offer a valuable option for managing advanced Parkinson’s disease and motor fluctuations. However, their use requires careful consideration and should be discussed thoroughly with healthcare professionals to ensure the most appropriate and effective treatment plan for the individual.
15. What are Rescue Therapies in Parkinson’s disease?
Apomorphine being used as a rescue therapy
Rescue therapies in Parkinson’s disease are interventions or strategies used to manage sudden and severe fluctuations in symptoms, often referred to as “off” episodes. These episodes occur when the effectiveness of standard Parkinson’s medications, particularly levodopa, diminishes, leading to a return of motor symptoms. Rescue therapies are designed to quickly and temporarily alleviate these off periods and improve motor function. Here are some commonly used rescue therapies:
- Apomorphine Subcutaneous Injection:
– Role: Apomorphine is a potent dopamine agonist that can be administered as a subcutaneous injection to rapidly improve motor symptoms during off periods.
– Administration: Given through a pre-filled injection pen.
– Onset of Action: Rapid onset, providing relief within minutes.
– Duration: Effects last for approximately one to two hours.
- Inhaled Levodopa (Inbrija):
– Role: Inbrija is an inhaled form of levodopa designed for on-demand use during off episodes.
– Administration: Inhaled through a handheld inhaler.
– Onset of Action: Rapid onset, providing relief within 10 minutes.
– Duration: Effects last for about 1-2 hours.
- Apomorphine Continuous Infusion:
– Role: Apomorphine can also be administered continuously through a portable infusion pump to provide a steady and continuous supply of dopamine.
– Administration: Subcutaneous infusion through a small needle.
– Onset of Action: Continuous dopaminergic stimulation.
– Duration: Can help reduce off periods throughout the day.
- Rescue Levodopa (Orally Disintegrating Tablets or Liquid Formulations):
– Role: Rapidly acting levodopa formulations, such as orally disintegrating tablets or liquid forms, can be used as rescue medications to provide quick relief during off periods.
– Administration: Administered orally or as a dissolvable tablet.
– Onset of Action: Faster onset compared to standard levodopa tablets.
– Duration: Short duration of action.
Considerations:
– Individualized Approach: The choice of rescue therapy depends on the individual’s specific needs, preferences, and response to medications.
– Adherence to Instructions: Proper training and education are essential to ensure correct administration of rescue therapies and optimize their effectiveness.
– Monitoring: Close monitoring of symptoms and response to rescue therapies is crucial for adjusting treatment plans as needed.
– Discussion with Healthcare Providers: Individuals with Parkinson’s disease and their healthcare providers should discuss the use of rescue therapies, including potential benefits and risks.
Rescue therapies play a valuable role in managing unpredictable and fluctuating symptoms in Parkinson’s disease, providing individuals with more control over their motor function during off periods. It’s important for individuals to work closely with their healthcare team to determine the most suitable rescue therapy and to receive proper guidance on its use.
16. What are the surgeries done for Parkinson’s Disease? Are they useful?
Apomorphine being used as a rescue therapy
Surgical interventions for Parkinson’s disease are considered when medication management alone is no longer sufficient in controlling symptoms, and the individual’s quality of life is significantly affected. These surgeries aim to alleviate motor symptoms by modulating specific areas of the brain. It’s important to note that surgery is not suitable for everyone, and the decision to undergo surgery is made on a case-by-case basis after thorough evaluation by a medical team. Here are two main types of surgeries used for Parkinson’s disease:
- Deep Brain Stimulation (DBS):
– Procedure: In DBS, electrodes are surgically implanted into specific areas of the brain, typically the subthalamic nucleus (STN) or the globus pallidus interna (GPi). These electrodes are connected to a pulse generator (similar to a pacemaker), which is implanted under the skin near the collarbone.
– Mechanism: The electrodes deliver electrical impulses to modulate abnormal neuronal activity and reduce motor symptoms.
– Effectiveness: DBS is often effective in improving motor fluctuations, reducing tremors, and enhancing overall motor control. It does not cure Parkinson’s disease but can provide significant symptom relief.
– Patient Selection: Suitable candidates for DBS are typically individuals with advanced Parkinson’s disease who have experienced motor complications despite optimal medication management.
- Lesioning Procedures:
– Procedure: Lesioning involves creating intentional, controlled damage to specific areas of the brain using techniques such as thalamotomy or pallidotomy.
– Mechanism: Lesioning procedures aim to interrupt abnormal neural circuits contributing to motor symptoms.
– Effectiveness: Lesioning procedures were more common before the advent of DBS. While they can provide symptom relief, they are irreversible, and DBS is often preferred due to its adjustable and reversible nature.
– Patient Selection: Lesioning procedures are less commonly performed today, and DBS is usually the preferred surgical option.
- Magnetic Resonance-Guided Focused Ultrasound (MRgFUS) Surgery:
– Procedure : MR-guided focused ultrasound (MRgFUS) is a non-invasive surgical technique that uses high-intensity focused ultrasound waves to create lesions or thermal ablations in targeted areas of the brain associated with Parkinson’s disease. It is an emerging technology that aims to provide therapeutic benefits without the need for traditional surgery or incisions.
– Mechanism : The targeted lesions disrupt or modulate neural circuits implicated in Parkinson’s disease, helping to alleviate motor symptoms
– Effectiveness: It is similar to lesioning surgeries except its non invasive. MRgFUS for Parkinson’s disease is an area of active research, and ongoing clinical trials are exploring its safety, efficacy, and long-term outcomes.
– Patient selection : MRgFUS is generally considered for individuals with Parkinson’s disease who have not responded adequately to medications and are not suitable candidates for other surgical interventions such as deep brain stimulation (DBS).
Considerations and Effectiveness:
– Individual Response: The effectiveness of surgical interventions can vary among individuals. Some experience significant improvement in motor symptoms, while others may see more modest benefits.
– Risk and Complications: Both DBS and lesioning procedures involve surgical risks, and there is a potential for complications such as infection or changes in mood or cognition. The benefits and risks are carefully weighed in the decision-making process.
– Medication Reduction: In some cases, surgical interventions may allow for a reduction in medication doses, helping manage medication-related side effects.
– Long-Term Outcomes: Long-term outcomes of surgical interventions for Parkinson’s disease are generally positive for appropriately selected candidates. Regular follow-up and adjustments are necessary to optimize outcomes over time.
Surgical interventions are considered when the benefits in terms of symptom control and quality of life outweigh the potential risks. It is crucial for individuals to have detailed discussions with their healthcare team to understand the potential benefits and risks associated with each surgical option and make informed decisions based on their specific circumstances.
17. How does exercise benefit Parkinson's patients?
Exercises for Parkinson Disease
Exercise can provide numerous physical and mental health benefits for individuals with Parkinson’s disease. While it does not cure the condition, regular exercise is recognized as an important component of Parkinson’s disease management. Here are several ways in which exercise can benefit Parkinson’s patients:
- Improved Motor Function:
– Increased Mobility: Exercise helps maintain and improve flexibility, balance, and coordination, which are often compromised in Parkinson’s disease.
– Reduced Rigidity: Physical activity can help alleviate muscle stiffness and improve overall movement.
- Enhanced Strength and Endurance:
– Muscle Strength: Resistance training and weight-bearing exercises contribute to increased muscle strength.
– Endurance: Aerobic exercises, such as walking or cycling, help improve cardiovascular fitness and overall stamina.
- Balance and Posture:
– Fall Prevention: Balance exercises reduce the risk of falls, a common concern for individuals with Parkinson’s disease.
– Improved Posture: Targeted exercises can help maintain a more upright posture.
- Motor Skills and Coordination:
– Fine Motor Skills: Activities that involve hand-eye coordination, like playing table tennis or practicing handwriting, can help maintain fine motor skills.
– Gross Motor Skills: Gross motor skills, such as walking and running, benefit from regular exercise.
- Neuroprotective Effects:
– Some studies suggest that exercise may have neuroprotective effects, potentially slowing the progression of Parkinson’s disease.
- Mood and Mental Well-being:
– Reduced Depression and Anxiety: Exercise is associated with improved mood and can help reduce symptoms of depression and anxiety.
– Stress Relief: Physical activity is a natural stress reliever, promoting overall mental well-being.
- Social Interaction:
– Participating in group exercises or classes fosters social interaction, reducing feelings of isolation.
- Cognitive Benefits:
– Some evidence suggests that exercise may have cognitive benefits, contributing to improved cognitive function in individuals with Parkinson’s disease.
- Medication Management:
– Regular exercise may enhance the effectiveness of medications used to manage Parkinson’s symptoms.
- Adaptability and Variety:
– Exercise programs can be adapted to an individual’s abilities and preferences, ensuring a personalized and enjoyable experience.
– Variety in exercises helps target different aspects of physical fitness.
Important Considerations:
– Consultation with Healthcare Professionals: Before starting any exercise program, individuals with Parkinson’s disease should consult with their healthcare team to ensure safety and appropriateness of the chosen activities.
– Individualized Approach: Exercise programs should be tailored to an individual’s abilities, taking into account their specific symptoms and needs.
– Consistency: Consistent, regular exercise is key to realizing the benefits. Aim for a combination of aerobic, strength, flexibility, and balance exercises.
– Enjoyment: Choosing activities that are enjoyable increases the likelihood of adherence to the exercise program.
Examples of suitable exercises for Parkinson’s patients include walking, cycling, swimming, yoga, tai chi, and strength training. The specific exercises should be chosen based on individual preferences and health status. Overall, exercise is a valuable and empowering tool for individuals with Parkinson’s disease, contributing to both physical and emotional well-being.
18. What are the risk factors for developing Parkinson's disease?
The exact cause of Parkinson’s disease is not fully understood, and it is likely influenced by a combination of genetic and environmental factors. While the majority of cases occur sporadically without a clear cause, certain risk factors have been identified that may contribute to the development of Parkinson’s disease. It’s important to note that having one or more risk factors does not guarantee the development of the disease, and individuals without these risk factors can still be diagnosed with Parkinson’s. Here are some recognized risk factors:
- Age:
– Risk Increases with Age: Parkinson’s disease is more commonly diagnosed in older individuals, and the risk increases with age. It is most often diagnosed in people over the age of 60.
- Genetics:
– Family History: While most cases of Parkinson’s disease are sporadic, having a first-degree relative (parent or sibling) with Parkinson’s may slightly increase the risk. Certain genetic mutations have been linked to familial or early-onset forms of the disease.
- Gender:
– Higher Incidence in Men: Men are slightly more likely than women to develop Parkinson’s disease.
- Environmental Exposures:
– Pesticides and Herbicides: Some studies have suggested a potential link between exposure to certain agricultural chemicals and an increased risk of Parkinson’s disease.
– Industrial Toxins: Exposure to certain industrial toxins, such as solvents and metals, has been explored as a possible risk factor.
- Head Trauma:
– Severe Head Injury: A history of significant head trauma, especially repeated injuries, has been associated with an increased risk of Parkinson’s disease.
- Rural Living:
– Living in Rural Areas: Some studies have indicated a higher incidence of Parkinson’s disease in individuals living in rural areas, possibly due to increased exposure to certain environmental factors.
- Smoking:
– Inverse Association: Some research has suggested that cigarette smoking may be associated with a lower risk of developing Parkinson’s disease. However, the health risks of smoking outweigh any potential protective effect.
- Caffeine Intake:
– Possible Protective Effect: Some studies have suggested a potential protective effect of caffeine, with individuals who consume coffee or tea having a slightly lower risk of developing Parkinson’s disease.
It’s important to recognize that the interplay between genetic and environmental factors is complex, and the exact mechanisms underlying the development of Parkinson’s disease are still being investigated. Additionally, research in this field is ongoing, and new insights may emerge over time. If individuals have concerns about their risk factors or are experiencing symptoms suggestive of Parkinson’s disease, it is advisable to consult with healthcare professionals for a thorough evaluation and guidance.
19. Can Parkinson's disease be prevented?
As of 2024, there is no known way to prevent Parkinson’s disease. The exact cause of Parkinson’s disease is not fully understood, and it likely involves a complex interplay of genetic and environmental factors. While certain risk factors have been identified, such as age, family history, and exposure to certain environmental toxins, it’s important to note that having one or more risk factors does not guarantee the development of Parkinson’s disease, and individuals without these risk factors can still be diagnosed with the condition.
Since the underlying mechanisms of Parkinson’s disease are not completely elucidated, prevention strategies are challenging. However, there are some lifestyle factors that have been suggested to potentially influence the risk of developing Parkinson’s disease, although more research is needed to establish conclusive evidence:
- Regular Exercise:
– Engaging in regular physical activity has been associated with a lower risk of developing Parkinson’s disease. Exercise may have neuroprotective effects and contribute to overall well-being.
- Healthy Diet:
– Adopting a healthy and balanced diet rich in antioxidants and nutrients may be beneficial for brain health. Some studies suggest that diets high in fruits, vegetables, and omega-3 fatty acids may have a protective effect.
- Avoiding Environmental Toxins:
– Minimizing exposure to certain environmental toxins, such as pesticides and industrial chemicals, has been suggested as a potential preventive measure. However, the evidence in this area is still evolving.
- Head Injury Prevention:
– Taking precautions to prevent head injuries may be important, as a history of severe head trauma has been linked to an increased risk of Parkinson’s disease.
It’s essential to emphasize that these lifestyle factors are not guaranteed preventive measures, and research in this area is ongoing. The focus of current medical approaches is on managing symptoms, improving quality of life, and exploring potential disease-modifying treatments
20. What is the latest research on Parkinson's treatment?
I can provide a general overview of some promising areas of research and potential avenues for Parkinson’s disease treatment that were being explored in the scientific community around that time. It’s important to note that the field of Parkinson’s research is dynamic, and new findings may have emerged since then. Here are some key areas of interest in Parkinson’s treatment research (as of 2024):
- Disease-Modifying Therapies:
– Researchers are actively seeking therapies that could slow or modify the progression of Parkinson’s disease, aiming to target the underlying neurodegenerative processes.
- Alpha-Synuclein Targeting:
– Alpha-synuclein is a protein that forms abnormal clumps (Lewy bodies) in the brains of people with Parkinson’s disease. Therapies targeting alpha-synuclein, such as antibodies and small molecules, are being investigated.
- Gene Therapies:
– Gene therapies, including the use of viral vectors to deliver therapeutic genes, are being explored as potential treatments. These approaches aim to address specific genetic or molecular factors associated with Parkinson’s disease.
- Stem Cell Therapy:
– Stem cell research is ongoing, exploring the potential of using stem cells to replace damaged or lost dopamine-producing neurons in the brains of individuals with Parkinson’s disease.
- Inflammation and Immune System Modulation:
– There is increasing interest in the role of inflammation and the immune system in Parkinson’s disease. Researchers are exploring therapies that modulate the immune response as a potential avenue for treatment.
- Focused Ultrasound:
– Focused ultrasound is being investigated as a non-invasive approach to treat Parkinson’s symptoms by targeting specific brain regions. This technique is under exploration for its potential to alleviate motor symptoms.
- Artificial Intelligence and Digital Biomarkers:
– Advances in artificial intelligence and digital health technologies are being applied to develop new biomarkers and diagnostic tools. These technologies may aid in early detection and monitoring of Parkinson’s disease.
- Exosome Therapy:
– Exosomes, small vesicles involved in cell-to-cell communication, are being explored as potential carriers for therapeutic molecules. This approach aims to deliver therapeutic agents to target cells in the brain.
- Microbiome and Gut-Brain Axis:
– Research is ongoing to understand the role of the gut microbiome in Parkinson’s disease. Some studies suggest a potential link between gut health and the development of Parkinson’s, opening new avenues for treatment exploration.
Clinical Trials:
– Many of these potential treatments are in various stages of preclinical and clinical trials. Participation in clinical trials is crucial for advancing research and testing the safety and efficacy of new therapies.
It’s important to check the latest scientific literature and clinical trial databases for the most recent developments in Parkinson’s disease research and treatment. Additionally, healthcare professionals and organizations such as the Michael J. Fox Foundation and Parkinson’s Foundation provide updates on ongoing research initiatives and breakthroughs in Parkinson’s disease.
21. Are there support groups for Parkinson's patients and caregivers?
Yes, there are numerous support groups available for individuals with Parkinson’s disease as well as their caregivers. These support groups offer a valuable platform for sharing experiences, exchanging information, and providing emotional support. Some of them are well know like Parkinsondotorg, APDA, and most countries have local support groups.
- American Parkinson Disease Association : https://www.apdaparkinson.org/
- Parkinson UK : https://www.parkinsons.org.uk/
- Parkinson Disease and Movement Disorders society (Local – India)
- Parkinson Disease Society of Karnataka (Local – State)
- Positive Attitude (Whatsapp group)
- Basal Ganglia Society (Local – State)
22. What is the prognosis for someone with Parkinson's disease?
The prognosis for someone with Parkinson’s disease can vary widely from person to person. Parkinson’s disease is a progressive neurodegenerative disorder, meaning that symptoms tend to worsen over time. However, the rate of progression and the specific symptoms experienced can differ significantly among individuals. Several factors influence the prognosis of Parkinson’s disease:
- Age at Onset:
– Generally, individuals diagnosed at a younger age may experience a longer disease course and potentially a slower progression of symptoms.
- Symptom Severity at Diagnosis:
– The severity of symptoms at the time of diagnosis can impact the overall prognosis. Some individuals may have milder symptoms initially, while others may experience more pronounced motor or non-motor symptoms.
- Response to Medication:
– A positive response to medications, particularly levodopa and other dopamine-replacement therapies, can help manage symptoms and improve quality of life. The effectiveness of medications can vary among individuals.
- Presence of Motor and Non-Motor Symptoms:
– The combination of motor symptoms (tremors, bradykinesia, rigidity) and non-motor symptoms (cognitive changes, mood disorders) can influence the overall prognosis.
- Treatment Adherence:
– Consistent adherence to prescribed medications and therapies can contribute to better symptom management and potentially slow the progression of the disease.
- Individual Health and Lifestyle Factors:
– Overall health, lifestyle choices, and the presence of other medical conditions can impact the progression and management of Parkinson’s disease.
- Advancements in Research and Treatment:
– Ongoing research into Parkinson’s disease may lead to new therapeutic approaches and interventions that could positively impact the prognosis in the future.
- Complications:
– Complications such as falls, infections, or other medical issues can affect the overall health and well-being of individuals with Parkinson’s disease.
It’s important to note that Parkinson’s disease is a chronic condition, and there is currently no cure. However, advancements in treatment options, including medications, surgical interventions, and various therapies, can significantly improve the quality of life for individuals with Parkinson’s disease.
As the disease progresses, some individuals may experience more advanced stages marked by increased challenges in mobility, cognition, and daily activities. In later stages, individuals may require more assistance with daily living activities.
23. Some Well known People / Personalities with Parkinson's Disease
Janet Reno
Janet Reno
The former U.S. Attorney General, Janet Reno, publicly disclosed her diagnosis of Parkinson’s disease in 1995. She served in the Clinton administration and passed away in 2016.
Billy Connolly
Billy Connolly
The Scottish comedian and actor, known for his distinctive humor, revealed his Parkinson’s diagnosis in 2013. He has continued to share his experiences with the disease in documentaries.
Estelle Getty
Estelle Getty
The actress, best known for her role as Sophia Petrillo on “The Golden Girls,” battled Parkinson’s disease in her later years until her passing in 2008.
Allan Border
Allan Border
Famous Australian Cricketer
Well Known Indians
Famous Indian People with Parkinson
There are well known people with Parkinson’s disease in India, however, most have chosen yet not to disclose to the public the diagnosis.
Michael J. Fox
Michael J. Fox
The Canadian actor and advocate is perhaps one of the most well-known figures associated with Parkinson’s disease. He was diagnosed with young-onset Parkinson’s in 1991 and has since become a prominent advocate for research and awareness
Muhammad Ali
Muhammad Ali
The legendary boxer Muhammad Ali was diagnosed with Parkinson’s disease in the 1980s, which was attributed to his boxing career. Despite his health challenges, he remained an influential figure until his passing in 2016.
Linda Ronstadt
Linda Ronstadt
The Grammy-winning singer revealed her Parkinson’s diagnosis in 2013, which ultimately led to her retirement from performing. She has since been outspoken about her journey with the disease.
Alan Alda
Alan Alda
The acclaimed actor best known for his role in “M*A*S*H” revealed in 2018 that he was diagnosed with Parkinson’s disease. He continues to be active in the entertainment industry and in raising awareness about the condition.
Neil Diamond
Neil Diamond
The iconic singer-songwriter Neil Diamond announced his Parkinson’s diagnosis in 2018, prompting him to retire from touring. He remains involved in music and philanthropy.
To Conclude
In conclusion, living with Parkinson’s disease requires a multidimensional approach, incorporating medical interventions, lifestyle adjustments, and a strong support network. The impact of the disease on daily life varies widely, influenced by factors such as age, symptom severity, and individual response to treatment. Despite the progressive nature of Parkinson’s disease, advancements in research and therapeutic strategies offer hope for improved outcomes and enhanced quality of life. Through ongoing dialogue with healthcare professionals, participation in support groups, and staying informed about the latest research, individuals with Parkinson’s and their caregivers can navigate the challenges of the disease with resilience and proactive management.
